In part 1 of this 2-part article we discussed ALT:AST ratio. In this article we will be talking about the reciprocal ratio, the AST:ALT Ratio also known as the DeRitis Ratio.
On the flipside… the ratio of AST to ALT, called the De Ritis ratio, can be calculated to monitor progression and severity of liver disease, and can also be used in the assessment of metabolic syndrome, muscle damage, and biliary obstruction. The AST:ALT ratio may become elevated over 1 in cirrhosis, muscle damage, biliary obstruction, and Wilson’s disease.[i] [ii] [iii] [iv] [v]
Liver disease
The AST:ALT ratio can assist in grading severity of pathology in chronic liver disease including alcoholic liver disease and chronic hepatitis. Increasing elevation of the AST:ALT ratio occurs as scarring and fibrosis progress due to tissue damage. An increasing ratio of AST to ALT above 1 is associated with progressive impairment of liver function and associated complications such as cirrhosis.[vi] Pharmaceutical drugs can cause liver damage as well, which in turn will be associated with an elevated AST:ALT ratio.
Liver detoxification and biotransformation is crucial to minimizing the toxic load on the body; it can be measured using the monoethylglycinexylidide (MEGX) test. Researchers observed an inverse correlation between MEGX results and AST:ALT ratio. MEGX values were significantly lower in those with an AST:ALT ratio of 1 or more, indicating impaired detoxification abilities.[vii]
In liver fibrosis, the AST:ALT ratio is especially useful because it can identify fibrosis even when both AST and ALT are within normal lab range. When the AST:ALT ratio rises above 1, fibrosis can be suspected, indicating that all is not normal.[viii]
Non-alcoholic fatty liver disease (NAFLD) without fibrosis or cirrhosis may be associated with an AST:ALT ratio below 1. The AST:ALT ratio is incorporated into a comprehensive NAFLD fibrosis score. A ratio of less than one is suggestive of NAFLD/non-alcoholic steatohepatitis. However, the ratio rises above 1 in 92% of alcoholic liver disease and climbs above 2 in 70% of cases.[ix]
Chronic hepatitis C without fibrosis is usually associated with an AST/ALT ratio less than 1.[x] However, in the event of fulminant acute viral hepatitis, AST may rise above ALT. In alcoholic hepatitis, AST is usually higher than ALT unless several days have passed without alcohol exposure at which time ALT may rise above AST. An increasing AST:ALT ratio in either condition may be a sign that long-term complications such as fibrosis and cirrhosis are occurring.[xi]
Alcohol abuse
Alcohol is intrinsically damaging to the liver and long-term consumption is associated with increased AST:ALT ratio once liver damage has set in. An AST:ALT ratio of 1.1 or less may be seen with alcohol abuse without cirrhosis. However, long-term alcohol abuse with cirrhosis was associated with an AST:ALT ratio of greater than 1.1. [xii]
In alcoholics with elevated aminotransferases, the mean AST:ALT ratio was 1.5 while for those with normal levels of individual aminotransferases, the ratio was 1.64.[xiii] With advanced alcohol abuse the ratio is often 2 or above.[xiv] The ratio may increase due to liver fibrosis or reduced clearance of AST by specialized liver cells called sinusoidal cells. [xv] Both AST and ALT enzymes require pyridoxal-5’-phosphate (vitamin B6) and its depletion, common in alcohol abuse, can reduce their levels, especially ALT.
Primary biliary cirrhosis (PBC) is characterized by portal inflammation and destruction of intrahepatic bile ducts and severity may be reflected in the ratio of AST to ALT. A statistically significant correlation was found between advanced PBC and increasing AST:ALT ratio.[xvi]
Biliary obstruction may cause an AST:ALT ratio of greater than 1.5 which suggests that intrahepatic cholestasis is likely. An AST/ALT ratio of less than 1.5 suggests extrahepatic obstruction.[xvii]
Muscle damage
An increasing AST:ALT ratio will be seen in muscle damage, as AST in muscle is significantly higher than ALT. The ratio is helpful in assessing critical limb ischemia (CLI), a form of peripheral artery disease disorder marked by severe obstruction of arteries in the extremities. An AST:ALT ratio of greater than 1.67 suggests a high risk of CLI.[xviii] An elevation of AST can be seen in myocardial infarction and calculation of the AST:ALT ratio may be helpful in assessing severity of cardiac muscle damage.[xix]
Metabolic syndrome risk factors such as waist circumference and waist-to-hip ratio, BMI, diastolic blood pressure, triglyceride levels, LDL, uric acid, fasting insulin levels, and insulin resistance were negatively correlated with ratio of AST to ALT in a random sample of 935 students ages 11-16. Researchers found that there was 6-fold greater risk of metabolic syndrome in those with the lowest AST:ALT ratios and central obesity was the most closely associated factor.[xx] A multicenter observational study of 1,625 adults confirmed that risk of metabolic syndrome was greatest in those with the lowest AST:ALT ratios.[xxi]
So, as you can see, elevated levels of AST and ALT and their ratio relationship can provide valuable clinical data.
| Condition | AST:ALT ratio |
| NAFLD in at-risk patients without liver fibrosis or cirrhosis | Less than 1 |
| Liver fibrosis | 1 or greater |
| Alcohol abuse without cirrhosis | 1.1 or less |
| Alcohol abuse with cirrhosis | Greater than 1.1 |
| Biliary obstruction, intrahepatic | Greater than 1.5 |
| Biliary obstruction, extrahepatic | Less than 1.5 |
| Critical limb ischemia in peripheral artery disease | Greater than 1.67 |
| Advancing cirrhosis | Greater than 2 |
| Advanced alcoholic liver disease | Greater than 3 |
Good news! The AST:ALT ratio is now being automatically calculated by the Optimal DX software if both the AST and ALT are added into the system. No need to do any conversions as the software will do this for you and will now show the result in the Blood Test Results Report:
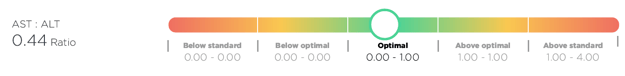
However, if you simply want to do the calculation manually then please follow these instructions:
The AST:ALT ratio is calculated by dividing the AST result by the ALT result.
Here's an example:
AST is 26 and the ALT is 22: 26 / 22 = 1.18
So, the AST:ALT Ratio in this example is 1.18

[i] Woreta TA, Alqahtani SA. Evaluation of abnormal liver tests. Med Clin North Am. 2014 Jan;98(1):1-16.
[ii] Thapa BR, Walia A. Liver function tests and their interpretation. Indian J Pediatr. 2007 Jul;74(7):663-71. Review. PubMed PMID: 17699976.
[iii] Rief P, Pichler M, Raggam R, et al. The AST/ALT (De-Ritis) ratio: A novel marker for critical limb ischemia in peripheral arterial occlusive disease patients. Medicine (Baltimore). 2016 Jun;95(24):e3843.
[iv] Hall P, Cash J. What is the real function of the liver 'function' tests? Ulster Med J. 2012 Jan;81(1):30-6.
[v] Gowda S, Desai PB, Hull VV, et al. A review on laboratory liver function tests. Pan Afr Med J. 2009 Nov 22;3:17.
[vi] Woreta TA, Alqahtani SA. Evaluation of abnormal liver tests. Med Clin North Am. 2014 Jan;98(1):1-16.
[vii] Giannini E, Risso D, Botta F, et al. Validity and clinical utility of the aspartate aminotransferase-alanine aminotransferase ratio in assessing disease severity and prognosis in patients with hepatitis C virus-related chronic liver disease. Arch Intern Med. 2003 Jan 27;163(2):218-24.
[viii] Newsome PN, Cramb R, Davison SM, et al. Guidelines on the management of abnormal liver blood tests. Gut. 2018 Jan;67(1):6-19.
[ix] Hall P, Cash J. What is the real function of the liver 'function' tests? Ulster Med J. 2012 Jan;81(1):30-6.
[x] Giannini E, Risso D, Botta F, et al. Validity and clinical utility of the aspartate aminotransferase-alanine aminotransferase ratio in assessing disease severity and prognosis in patients with hepatitis C virus-related chronic liver disease. Arch Intern Med. 2003 Jan 27;163(2):218-24.
[xi] Botros M, Sikaris KA. The de ritis ratio: the test of time. Clin Biochem Rev. 2013 Nov;34(3):117-30. Review.
[xii] Botros M, Sikaris KA. The de ritis ratio: the test of time. Clin Biochem Rev. 2013 Nov;34(3):117-30. Review.
[xiii] Kawachi I, Robinson GM, Stace NH. A combination of raised serum AST:ALT ratio and erythrocyte mean cell volume level detects excessive alcohol consumption. N Z Med J. 1990 Apr 11;103(887):145-8.
[xiv] Lala V, Goyal A, Bansal P, Minter DA. Liver Function Tests. 2020 Mar 27. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-.
[xv] Thapa BR, Walia A. Liver function tests and their interpretation. Indian J Pediatr. 2007 Jul;74(7):663-71. Review.
[xvi] Alempijevic T, Krstic M, Jesic R, et al. Biochemical markers for non-invasive assessment of disease stage in patients with primary biliary cirrhosis. World J Gastroenterol. 2009 Feb 7;15(5):591-4.
[xvii] Hall P, Cash J. What is the real function of the liver 'function' tests? Ulster Med J. 2012 Jan;81(1):30-6.
[xviii] Rief P, Pichler M, Raggam R, et al. The AST/ALT (De-Ritis) ratio: A novel marker for critical limb ischemia in peripheral arterial occlusive disease patients. Medicine (Baltimore). 2016 Jun;95(24):e3843. doi: 10.1097/MD.0000000000003843. Erratum in: Medicine (Baltimore). 2016 Aug 07;95(31):e5074.
[xix] Rej R. Aminotransferases in disease. Clin Lab Med. 1989 Dec;9(4):667-87. PMID: 2686908.
[xx] Lin S, Tang L, Jiang R, et al. The Relationship Between Aspartate Aminotransferase To Alanine Aminotransferase Ratio And Metabolic Syndrome In Adolescents In Northeast China. Diabetes Metab Syndr Obes. 2019 Nov 18;12:2387-2394
[xxi] Hanley AJ, Williams K, Festa A, et al. Liver markers and development of the metabolic syndrome: the insulin resistance atherosclerosis study. Diabetes. 2005 Nov;54(11):3140-7.